Pictures of common skin rashes, symptoms & treatments
No one wants to scratch an itch only to discover that a red, bumpy rash has cropped up, but the truth is that we’re all bound to get a rash at some point or another.
Luckily, rashes are common occurrences and can be treated relatively easily with the right knowledge and care.
Below, we’ll review different kinds of rashes and rash pictures to help you become familiar with some of the most common types of skin rashes, what you can do about them, and when you should see a doctor.
Common rash pictures: Know what to look for
Here are some of the most common types of skin rashes. We’ve included common characteristics and treatment options for each condition, plus pictures of the rashes to help you identify and differentiate between them.
Eczema
Atopic dermatitis, also known as eczema, is a non-contagious skin condition that’s characterized by itchy, red, and dry skin. According to the National Institute of Allergy and Infectious Diseases (NIAID), eczema affects nearly 30 percent of the U.S. population.
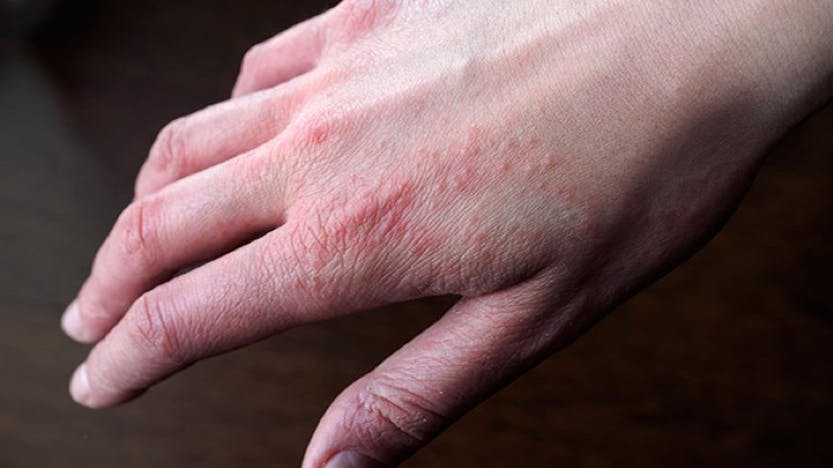
Source: Everyday Health
Unfortunately, eczema isn’t curable, but it is treatable. For many, the most effective short-term treatment is applying an anti-itch cream or a rich moisturizer and/or taking an oral allergy medication.
For eczema sufferers who can’t find relief through at-home methods, more powerful prescription topical and oral medications exist, such as hydrocortisone cream and Diphenhydramine (Benadryl), respectively.
If the patient’s affected skin has contracted a secondary infection, antibiotics may also be necessary.
Poison ivy, poison oak, and sumac rashes
Poison ivy, poison oak, and sumac are plants that can cause redness, blotchy spots, itching, blisters, and/or swelling upon contact.
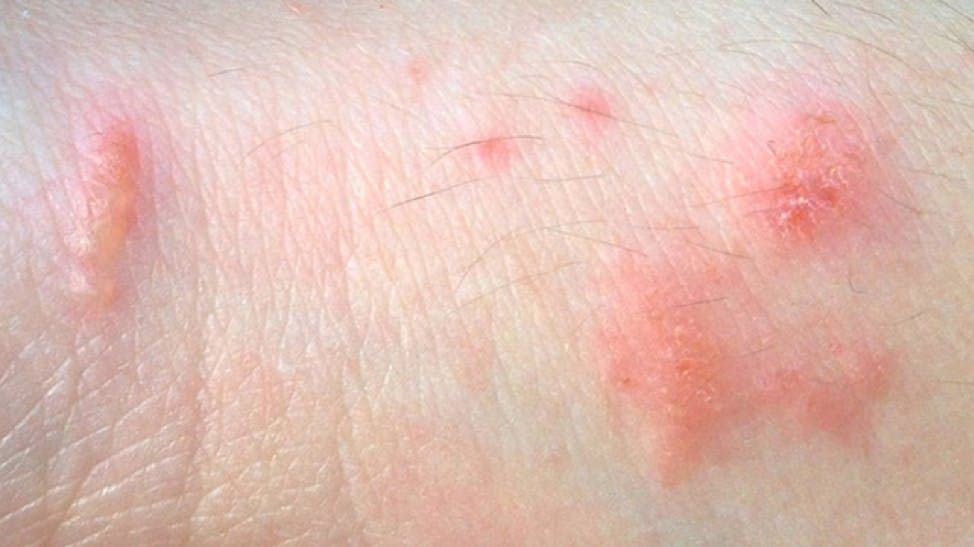
According to Mayo Clinic, poison ivy, poison oak, and sumac rashes are caused by urushiol, an oily resin that coats the plants.
Although washing your skin immediately after exposure can help reduce your risk of getting a rash, the urushiol's oily nature can make it difficult to wash off.
Over-the-counter washes designed to target urushiol can be purchased at drugstores, but if you’re not able to use such a wash before the rash sets in, there’s little you can do besides treating the worst of the rash’s symptoms.
To soothe poison ivy, poison oak, and sumac rashes, many turn to non-prescription anti-itch creams, which can help reduce itching. Other home treatments include cold compresses and oatmeal baths.
People with severe rashes, blistering, and swelling should see a medical provider and may be prescribed a topical treatment.
Scabies
Unlike superficial rashes, scabies is caused by microscopic burrowing mites that infest and lay eggs in the outer layers of the skin.
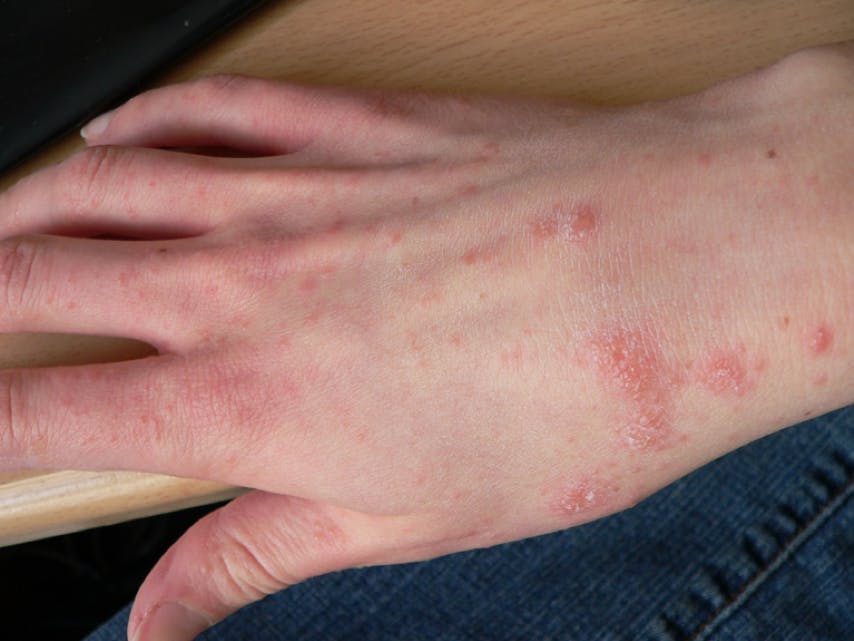
According to the Centers for Disease Control and Prevention (CDC), scabies is usually spread through skin-to-skin contact with infected persons. Its most common symptoms are severe itching and a pimple-like rash, though tiny burrows can sometimes be seen with the naked eye.
Scabies is far from uncommon — the American Academy of Dermatology states that there are millions of cases worldwide each year.
Scabies mites can live for up to two months in a person’s skin, so scabies rashes won’t simply go away on their own in a short amount of time.
Currently, the only treatment for scabies is a topical prescription, which must be obtained through a medical provider — no over-the-counter treatments exist.
Psoriasis
According to the National Psoriasis Foundation, psoriasis is a non-contagious skin condition that’s characterized by a red, bumpy, and/or scaly rash.
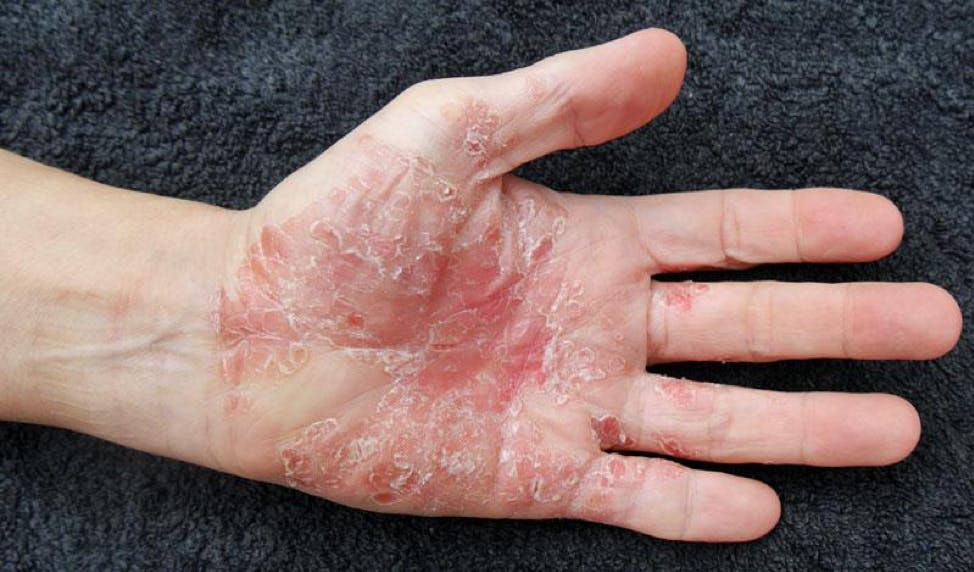
Psoriasis rashes are often accompanied by burning, itching, and stinging sensations. There are several types of psoriasis, with the most common being plaque psoriasis, which is identifiable by its silvery-white, dry, and itchy rashes.
For mild cases of psoriasis, over-the-counter moisturizers, ointments, and creams can provide relief.
For more severe cases or a particularly bad flare-up, prescription-strength topical and oral medications can be provided by a medical provider.
Tick bites
Ticks are small, bloodsucking parasites that populate every U.S. state in the form of one or more species, according to the CDC. Tick bite rashes can appear as a small red dot or can grow to resemble a large red bullseye.
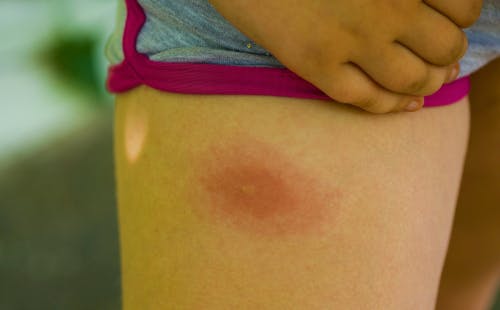
Since ticks burrow their head into the skin of their host, they will remain attached until they are engorged with blood or forcefully removed. The CDC recommends removing ticks with a pair of fine-tipped tweezers, taking care to apply steady, even pressure without twisting or jerking.
Improper removal can cause the tick’s head or mouthparts to remain embedded in the skin. If those can’t be removed with tweezers, it’s necessary to seek medical attention to avoid an infection.
Red bullseye-shaped rashes like the one in the image above can be an indication that the tick has transmitted Lyme disease, a disease that can cause both short- and long-term symptoms such as fatigue, headache, chills, swollen lymph nodes, and other flu-like symptoms.
To treat early-stage Lyme disease, patients are typically prescribed oral antibiotics, while late-stage Lyme disease can be treated with intravenous antibiotics, according to the Canadian Lyme Disease Foundation. No over-the-counter treatments for Lyme disease are currently available.
Ringworm
Ringworm is a fungal skin infection. According to the Mayo Clinic, ringworm can trigger an itchy, circular, or ring-shaped rash caused by direct contact with another infected individual’s skin.
The same type of fungus that causes ringworm is responsible for jock itch, which is a fungal infection in the groin region. It also causes athlete’s foot, which is a fungal infection that usually occurs between the toes.
Most cases of ringworm are relatively mild and easily treated with non-prescription topical anti-fungal creams, sprays, or powders such as clotrimazole or miconazole. You should see a doctor if an over-the-counter anti-fungal doesn’t clear up symptoms after using it as directed, as a stronger anti-fungal may be needed.
Chickenpox
Chickenpox is a highly contagious viral infection that causes an itchy, blistering rash. A fever and fatigue may also accompany the rash. The blisters tend to be small, round, and fluid-filled.
According to the Mayo Clinic, the chickenpox rash is a three-stage cycle. The rash begins as raised, red bumps, which then fill with fluid and burst. Finally, the blisters dry out, scab over, and begin to heal.
Treatment for chickenpox includes various at-home therapies to relieve itching and discomfort, such as oatmeal baths, calamine lotion, and over-the-counter antihistamines. It’s essential to resist scratching a chickenpox rash to prevent scarring and bacterial skin infections.
Seasonal rashes
Although rashes can appear at any time of year, some are more frequently seen during certain seasons. Here are the most common rashes for each season, some of which we’ve covered in this article:
Winter
The cold, dry air of winter can contribute to dry, cracked skin. The lack of humidity in the environment can worsen symptoms of some types of skin rashes. These include:
- Eczema
- Psoriasis
Spring
Spending more time outdoors during spring and summer means rashes related to plants, insects, and sun exposure are more common during these seasons.
Common spring skin rashes include:
- Drug-induced photosensitivity occurs when a drug combines with sunlight to produce irritation or an allergic reaction.
- Heat rash, which is a red, blistery rash caused by trapped sweat.
- Lyme disease
- Pityriasis rosea, which is a patchy, widespread rash that can linger for months.
- Poison ivy, oak, and sumac
- The polymorphous light eruption is a raised, bumpy rash that’s caused by exposure to sunlight in some people.
Summer
The types of rashes common in spring are often seen during the summer, including:
- Drug-induced photosensitivity
- Heat rash
- Lyme disease
- Poison ivy, oak, and sumac
- Polymorphous light eruption
The heat of summer and many summer environments can also lead to the following skin conditions:
- Chronic rashes
- Eczema
- Hives are an outbreak of swollen, red, and itchy welts that form in response to an allergen or irritant.
- Insect bites and stings, such as mosquito bites or bee stings.
- Swimmer’s itch, which is a rash caused by burrowing parasites that are found in warm bodies of water.
Fall
Fall allergies and the cooler temperatures of fall can lead to an increase in:
- Hives
- Allergic reactions
- Eczema and psoriasis
- Pityriasis rosea
Rashes on babies & children
Several childhood illnesses cause different kinds of rashes. The following conditions are seen mostly in babies and children.
Fifth disease
The fifth disease is a viral infection caused by parvovirus. According to the CDC, the infection results in a red rash on the cheeks of the face, known as a “slapped cheek” rash. The rash can be present on other parts of the body, but the cheek rash is the most common.
Other symptoms include fever, runny nose, sore throat or headache. Some people experience joint pain or swelling, as well.
Other than managing symptoms with over-the-counter medications, there is no treatment or recommended medication for Fifth disease. Most cases of Fifth disease are mild and resolve on their own.
Impetigo
Impetigo is a bacterial infection of the skin. It causes the affected skin to break out in red, fluid-filled sores, which itch, leak, and eventually scab over and heal. The infection requires a doctor’s diagnosis and can be easily treated with oral and/or topical antibiotics.
Hand, foot, and mouth disease
Hand, foot, and mouth disease is a highly contagious viral infection that primarily affects children under the age of five.
Symptoms include sores inside the mouth, rash on the bottoms of the feet and palms of the hands, and fever. The rash looks like small, red, flat dots. It doesn’t itch, but it may blister and scab over.
There is no treatment for hand, foot, and mouth disease. At-home comfort measures, such as over-the-counter medication, can be used to manage fever and discomfort caused by sores.
Diaper rash
Young children still in diapers are prone to diaper rash. This rash is a form of dermatitis that causes red, inflamed skin in the diaper region, including the buttocks, genitals, and thighs. It’s often tender and may be warm to the touch.
More frequent diaper changing and over-the-counter medications typically clear up diaper rash in a few days. More complicated cases may require a doctor’s prescription.
Scarlet fever
When strep throat presents with a rash, it is scarlet fever. According to the CDC, the bacteria that cause strep throat can produce a toxin that causes a skin rash. The rash can appear anywhere on the body and starts as a red flush that turns into a rough, bumpy texture.
A doctor can administer a strep test to diagnose scarlet fever, and antibiotics are prescribed to treat the infection.
Other rashes to be aware of
Rosacea
Rosacea is a chronic skin condition that causes redness or flushing on the face. Small, red bumps may also be present.
People with this condition tend to experience flares that come and go. The Mayo Clinic lists heat, spicy foods, alcohol, stress, and sunlight as triggers for rosacea flare-ups. There is no cure, and avoiding triggers is the best way to manage flares.
Dermatitis
There are two types of dermatitis: atopic dermatitis (eczema) and contact dermatitis. Contact dermatitis is acute and caused by contact with an irritant or allergen.
Contact dermatitis can be very red and inflamed and can occur on any part of the skin that contacts the irritant. It may or may not itch or be tender.
Avoiding the irritant that caused the rash and using over-the-counter medications can help relieve discomfort.
Shingles
The virus that causes chickenpox causes shingles. Shingles present as a painful rash that may or may not blister. If blisters are present, they eventually leak and scab over. The rash appears in one area of the body, usually on one side of the torso or face. Pain and tingling may occur before the rash appears or persist once the rash subsides.
Antiviral medications may shorten the duration of shingles, and at-home measures, like calamine lotion and oatmeal baths, may help soothe irritated skin.
Measles
Measles is a highly contagious respiratory virus that causes fever and a skin rash. The rash begins at the top of the body and spreads downward.
Lab testing is required to diagnose measles. There is no cure or treatment for measles.
Visit urgent care to identify skin rashes
Though some rashes can be successfully identified and treated by comparing the rash on your skin to the pictures provided here, some types of skin rashes must receive medical attention.
You should see a medical provider if your rash:
- Covers all or most of your body.
- Came on suddenly and spread rapidly.
- Is accompanied by a fever or flu-like symptoms.
- Begins to blister.
- Is causing pain.
- Appears to be infected.
- Is shaped like a bullseye.
- Isn’t showing signs of improvement after a few days.
- Is unresponsive to over-the-counter treatments.
- Is accompanied by symptoms of a severe allergic reaction, like difficulty breathing or severe swelling.
- Is accompanied by an uncontrollable itch, as scratching can lead to infection.
An ongoing rash can also be an indication of a chronic skin condition and should be examined by a medical professional.
If you have a rash that needs medical attention or simply want to treat your rash, a visit to one of the urgent care locations can give you the relief you need. You can walk in, or save your spot online.
*Disclaimer: This information is not intended to serve as medical advice. Please visit your local urgent care center to receive a proper medical diagnosis for your rash.
Written by Sarah Thebarge, Physician Assistant


